Return to Football After Sciatica-Related Back Pain
Patient:
Sandra, 35-year-old recreational footballer
Sandra presented to Total Body Physio with persistent lower back and left leg pain that had forced her to stop playing football and was beginning to interfere with work, sleep, and daily activities.


Sandra’s Story
Clinical assessment identified:
- Restricted, symptom-provoking lumbar flexion and left rotation
- Positive left-sided neural tension testing
- Poor gluteal activation on prone hip extension
- Reduced gluteus medius stability and trunk control during single-leg stance and squat
- Paraspinal guarding and tenderness at L4/5–L5/S1 with partial leg pain reproduction
- Normal neurological screening with no red flags for urgent imaging
Interpretation: Findings were consistent with lumbar-related leg pain with neural mechanosensitivity, commonly termed sciatica, without signs of significant nerve root compression. Positive neurodynamic tests are associated with neural sensitivity and may help identify patients who respond well to movement-based rehabilitation (Childs et al., 2021).
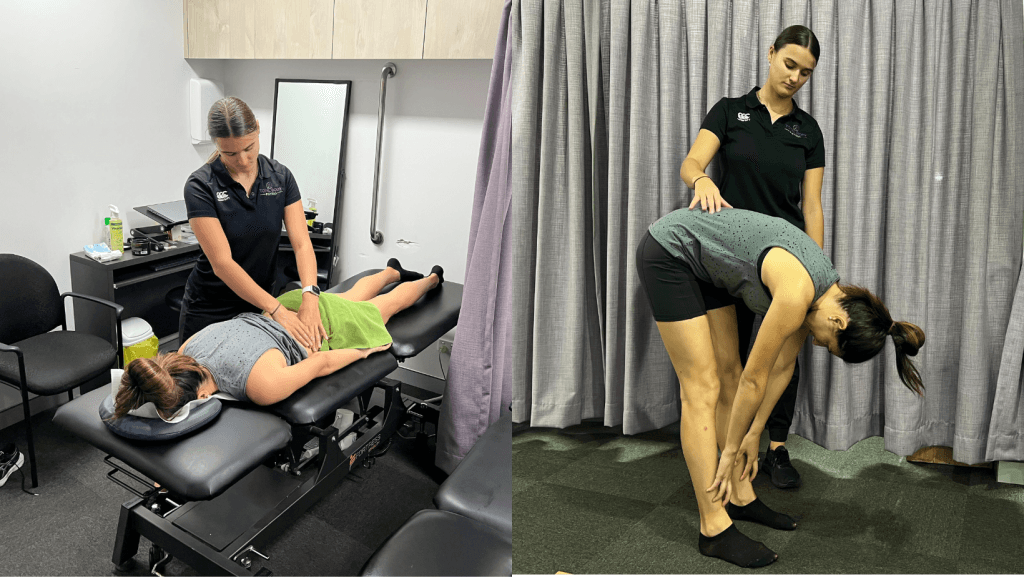

Understanding Sciatica
Sciatica describes leg pain arising from irritation or sensitisation of lumbar nerve roots or adjacent neural tissue. Current evidence suggests symptoms are often influenced by load management, movement patterns, and neuromuscular control rather than structural injury alone (Lewis et al., 2021).
Football places high demands on the lumbar spine through sprinting, rotation, kicking, and rapid changes of direction. Rapid load increases or inadequate recovery may exceed tissue capacity/tolerance and contribute to neural sensitivity (York et al., 2020). Current evidence supports graded exposure and progressive loading over prolonged rest (O’Sullivan et al., 2020).
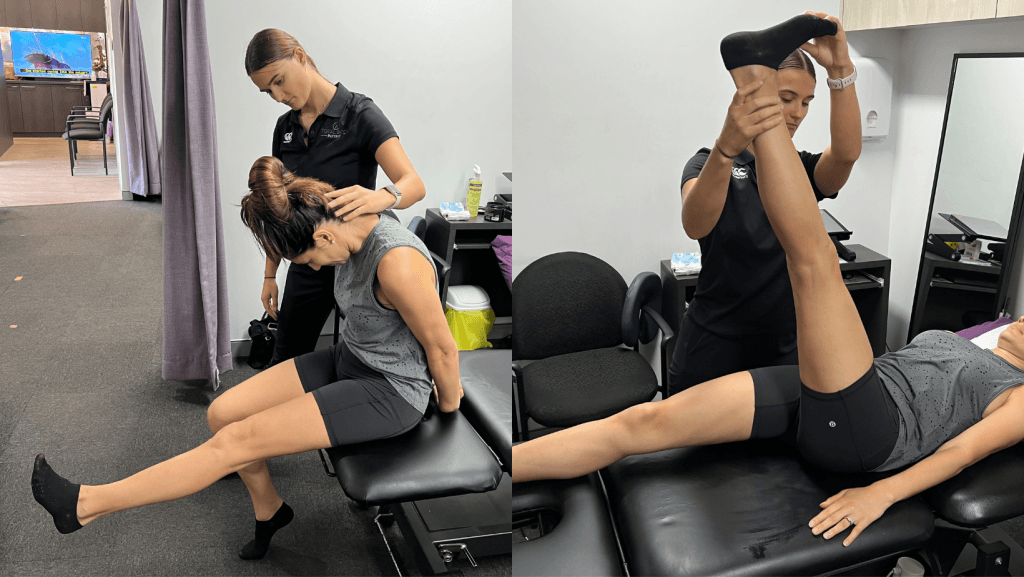

Imaging Considerations
Guidelines emphasise clinical and functional assessment over routine imaging when red flags are absent, aligning with evidence that physical signs and movement responses are more prognostic than radiological findings (Maher et al., 2021). MRI findings such as disc bulges or foraminal narrowing are common in asymptomatic populations and do not reliably predict pain or recovery trajectory (Jensen et al., 2020). Sandra was therefore not referred for imaging.
The Plan
Rehabilitation aimed to restore tolerance to football-specific load while addressing movement impairments, neural sensitivity, and strength deficits.
Early Phase
Goals: Reduce neural irritation and improve baseline control without exacerbating pain.
- Temporary pause from football with modification of prolonged sitting and repetitive bending (Apeldoorn et al., 2024)
- Manual therapy, gentle lumbar mobility, gentle stretching and pain-free neural mobilisation to reduce symptoms and improve movement tolerance (Peacock et al., 2022)
- Education emphasising that movement is safe, that symptoms reflect sensitivity rather than damage, and that gradual loading improves long-term outcomes (Traeger et al., 2022)
- Early trunk, gluteal, and pelvic stability exercises were introduced. Early activation of transverse abdominis and multifidus aims to reduce fear-avoidance and improve control (Smith et al., 2023)
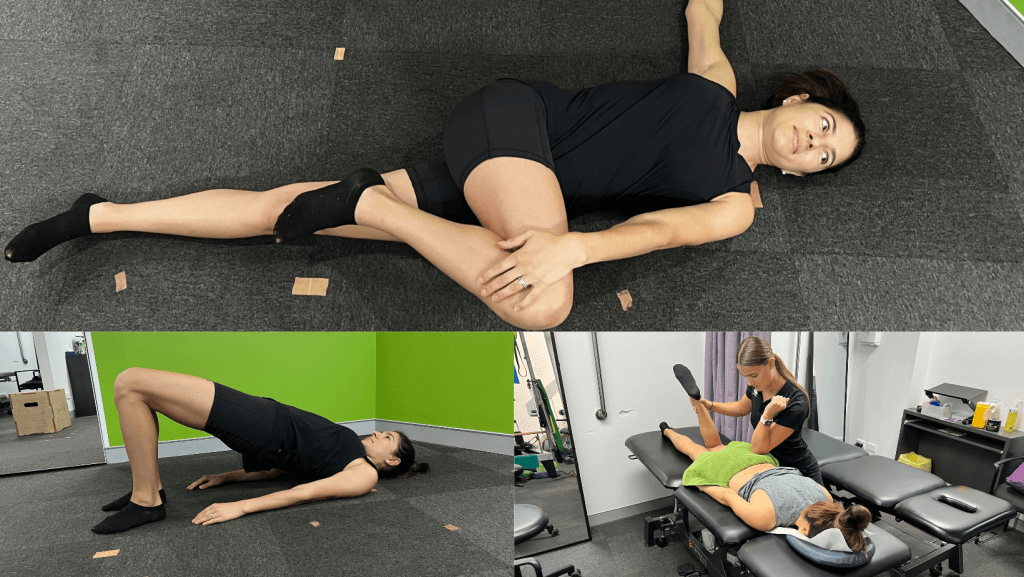

Progression Phase
Goals: Increase strength, dynamic control, and sport-specific capacity.
- Segmental and global strengthening of hips and trunk were progressed based on tolerated load. Gym-based exercises including squats, deadlifts, RDLs, and lunges, were included, as were global exercises for her lower limb targeting a return to football. High-volume strength training has been linked with better functional outcomes and reduced recurrence of back-related leg pain (Jones et al., 2022).
- Clinical Pilates on reformer focusing on trunk and pelvic control, endurance, and coordination was included as it’s shown to improve core stability and functional outcomes in back pain populations (Silverio et al., 2022)
- Gradual reintroduction of agility, acceleration, and change-of-direction drills were included exposing neural tissues to sport loads. Progressive sport-specific training has been correlated with faster return-to-sport times compared with generic conditioning (Murphy et al., 2021).
- Criteria-based progression guided by movement quality, strength benchmarks (AxIT limb symmetry above 85%), and symptom response rather than elapsed time alone is associated with improved return-to-play readiness and lower reinjury rates (Anderson et al., 2021)


Progress and Outcome
Across seven weeks Sandra demonstrated measurable improvement:
- Sitting tolerance increased from ~20 minutes to over 90 minutes by week four
- Gluteal strength improved to within 10 percent side-to-side difference
- Symptom-free single-leg hop and cutting tasks with good control
- Full team training resumed by week six with minimal stiffness
- Unrestricted match play by week seven with strong self-management confidence
These outcomes align with evidence that early active rehabilitation combined with graded sport re-introduction is associated with faster return and lower recurrence compared with passive care alone (Stanton et al., 2022).
Key Clinical Takeaways
- Lumbar-related leg pain often reflects neural sensitivity influenced by movement and load tolerance, not solely structural findings
- Neurodynamic and functional testing assist in identifying suitable candidates for movement-based rehabilitation
- Education and load management strategies are linked with reduced disability and improved confidence
- Targeted hip and trunk strengthening supports spinal control and recurrence reduction
- Criteria-based return to sport is associated with stronger functional outcomes than time-based progression
Sandra’s case highlights how evidence-informed assessment, personalised load management, and progressive, criteria-based rehabilitation may support safe return to sport following sciatica-related symptoms.
If you or someone you care for has an injury, a flare up, requires some rehabilitation or experiences an increase in pain, give the clinic a call on 9713 2455 or book online.